Progress Report Template For Construction Project. Creative and colourful components create this vibrant template that is sensible and fascinating. Enjoy full entry to a contemporary, cloud-based vulnerability administration platform that enables you to see and track your whole belongings with unmatched accuracy. A template for a disciplinary or grievance investigation report. Send Acas templates for a disciplinary or grievance investigation plan and a disciplinary or grievance investigation report. Drawing on extensive consultations throughout the LP and GP communities and with technical experts, on January 29, 2016, the ILPA released the ILPA Reporting Template for charges, bills, and carried curiosity. Attachment C, Market Research Report Template, of the DHS Market Research Guide provides a pattern market analysis report template that can be tailored to specific market analysis wants.
The many infographics and the brilliant yellow colour make this annual report design fascinating and distinctive. Use report templates to create reports with views in your scan outcomes and the current vulnerabilities on your hosts. You can choose an current Progress Report Template For Construction Project we provide as a place to begin, or you probably can create custom stories by telling us all the settings. Daily Management Report and Performance Log FormIf you search day by day efficiency and administration report type, you don’t want to search more.
You don’t want them to be distracted by the design parts. One of the core elements that you are going to wish to edit in your annual report template is the textual content. Regardless of what program you’re utilizing, text editing is very easy to do. Let’s have a glance at some fast suggestions that can help you begin customizing your annual report template right now. For this demonstration, we’ll work with an annual Progress Report Template For Construction Project for Adobe InDesign. These processes will differ if you choose to use a unique software surroundings.
Specifically, the white background, the orange details and the dot elements, make this annual report unforgettable. Choose to inform your business’s story with the help of this elegant annual report. The shade palette is subtle, the overall layout is creative, and the construction is flawless. Organize your data from the earlier yr and showcase your achievements and growth with this elegant annual report template. An annual report design such as this one is trendy, yet timeless. This Progress Report Template For Construction Project in particular, contains a lot of graphical data, charts, and paragraphs that permit you to successfully inform your story.
Grab the attention of your managers by telling a story together with your knowledge. Whether you’re reporting on how you’re performing, what quantity of sales you made this month, or how your business is performing, our templates are tremendous simple to make use of. Just choose one, add in your personal knowledge, images, and text, and ship the report to your boss or print it out. Free annual report templates are an excellent place to begin, however they’ve their shortcomings. These free annual report templates haven’t got all of features that premium templates have. But let’s say you are simply on the lookout for one, particular asset.
Creating stories is time-consuming sufficient with out having to fret about graphic design as nicely. Daily Field Report FormAre you a supervisor that wishes to trace how workers spend their time and behave whereas working outside? This day by day field Progress Report Template For Construction Project will allow you to verify whether an employee had attended the on-site job for your client.
Make Stunning Progress Report Template For Construction Project
To help make your report extra fascinating and more full, ensure to include images. Images that are associated to the page that you just’re on in your report give your reader a break from the entire dense information that you’ll be presenting. While using popular colours like blue have a desired impression in your viewers, utilizing shiny colours is also acceptable. Bright colours actually pop out of the page and may make your presentation seem extra vigorous. This can positively help when you’re presenting dense material in your annual report. Use company colours, fonts, and other model belongings all through the report to hold it on model.
Just fill in key stats to elucidate your progress and prove your work is delivering results. A report template also can save you time and hold revisions to a minimal and is available in quite so much of formats of report styles. You’ll discover you presumably can cut your writing time in half with a available MLA or APA template format. Create and present your info with our well-structured and attention-grabbing report templates. These professionally designed report templates are free and simple to make use of. Find a Progress Report Template For Construction Project that most intently fits your business or customize it as necessary.
Envato Elements and GraphicRiver are two excellent choices for premium, skilled designs at a aggressive value. More typically than not, you’ll want to change the colors within your annual report template to match your brand. Regardless of what software program you select to edit the Progress Report Template For Construction Project, the first step is to look at all of the pages included within the template. That means you can find the exact pages that can fit your explicit annual report template. If you prefer working with PowerPoint, give this report template free download a try. Another place to seek out premium annual report templates is GraphicRiver.
Gallery of Lovable Progress Report Template For Construction Project
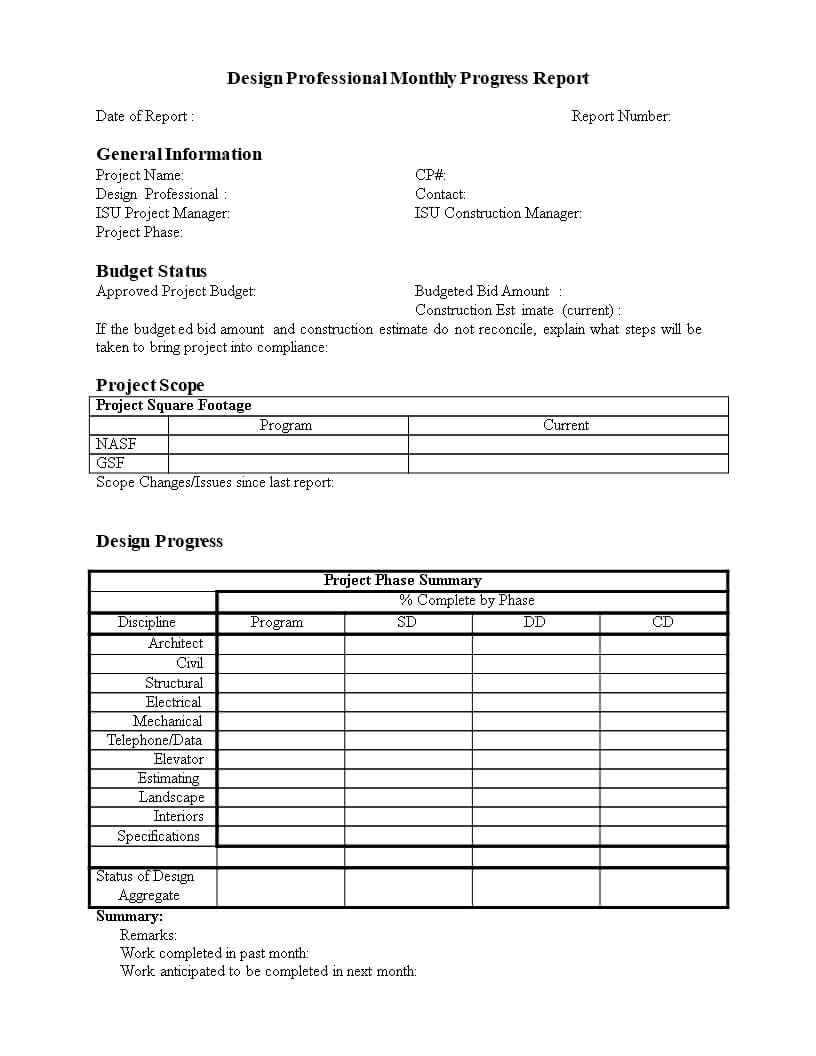
Monthly Progress Report In Word | Templates At within Progress Report Template For Construction Project
Project Progress Report Template E2 80 93 Wovensheet Co for Progress Report Template For Construction Project
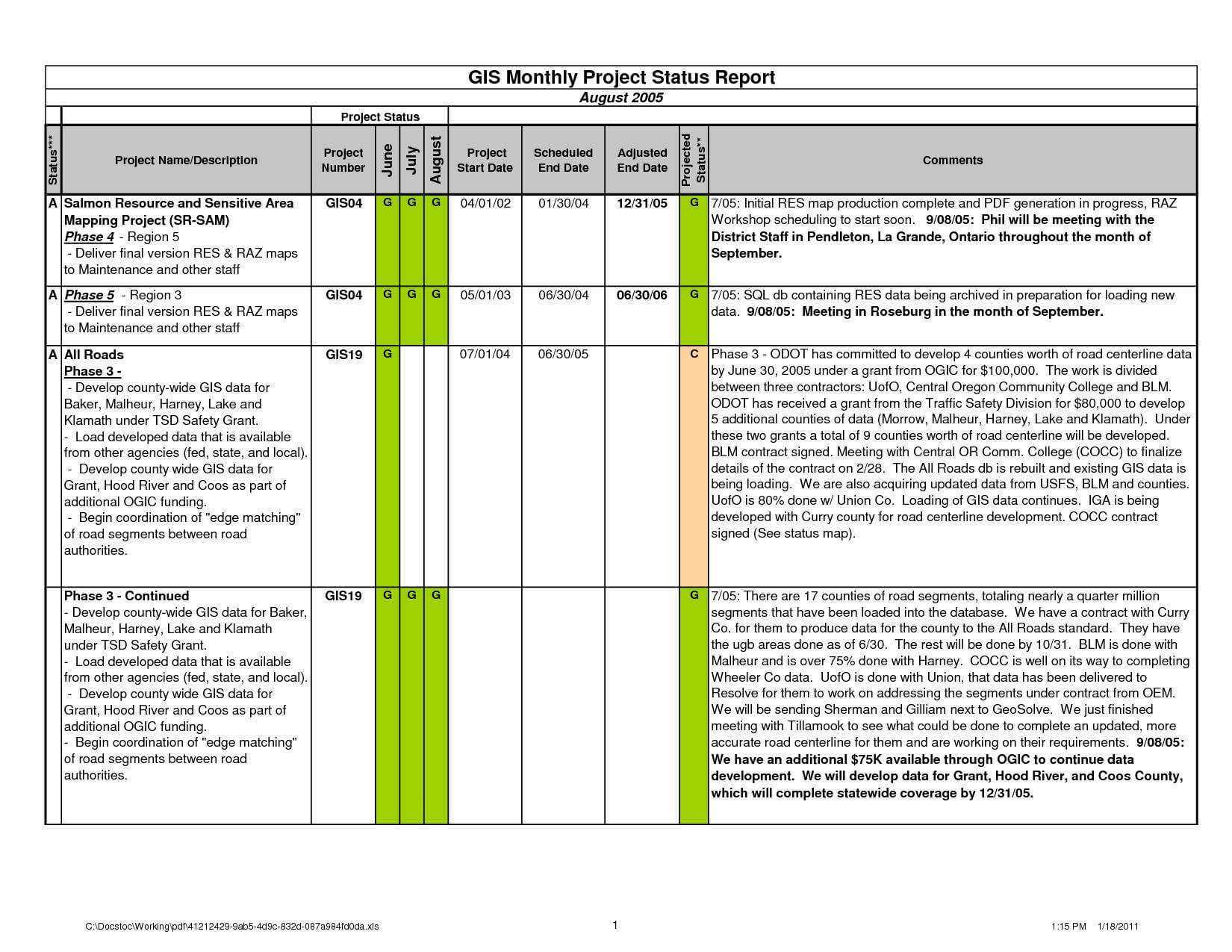
Construction Project Report Sample Progress Download with regard to Progress Report Template For Construction Project
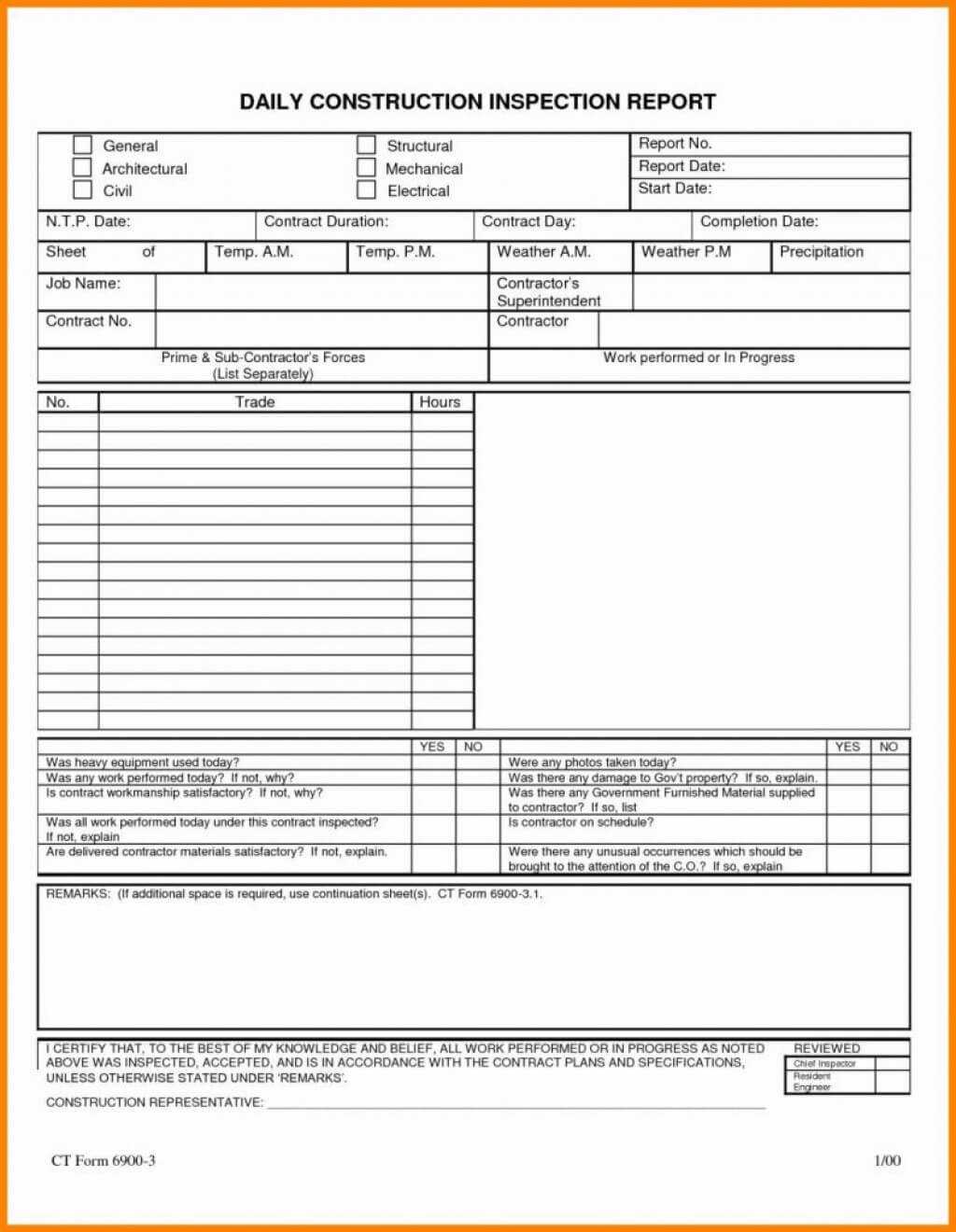
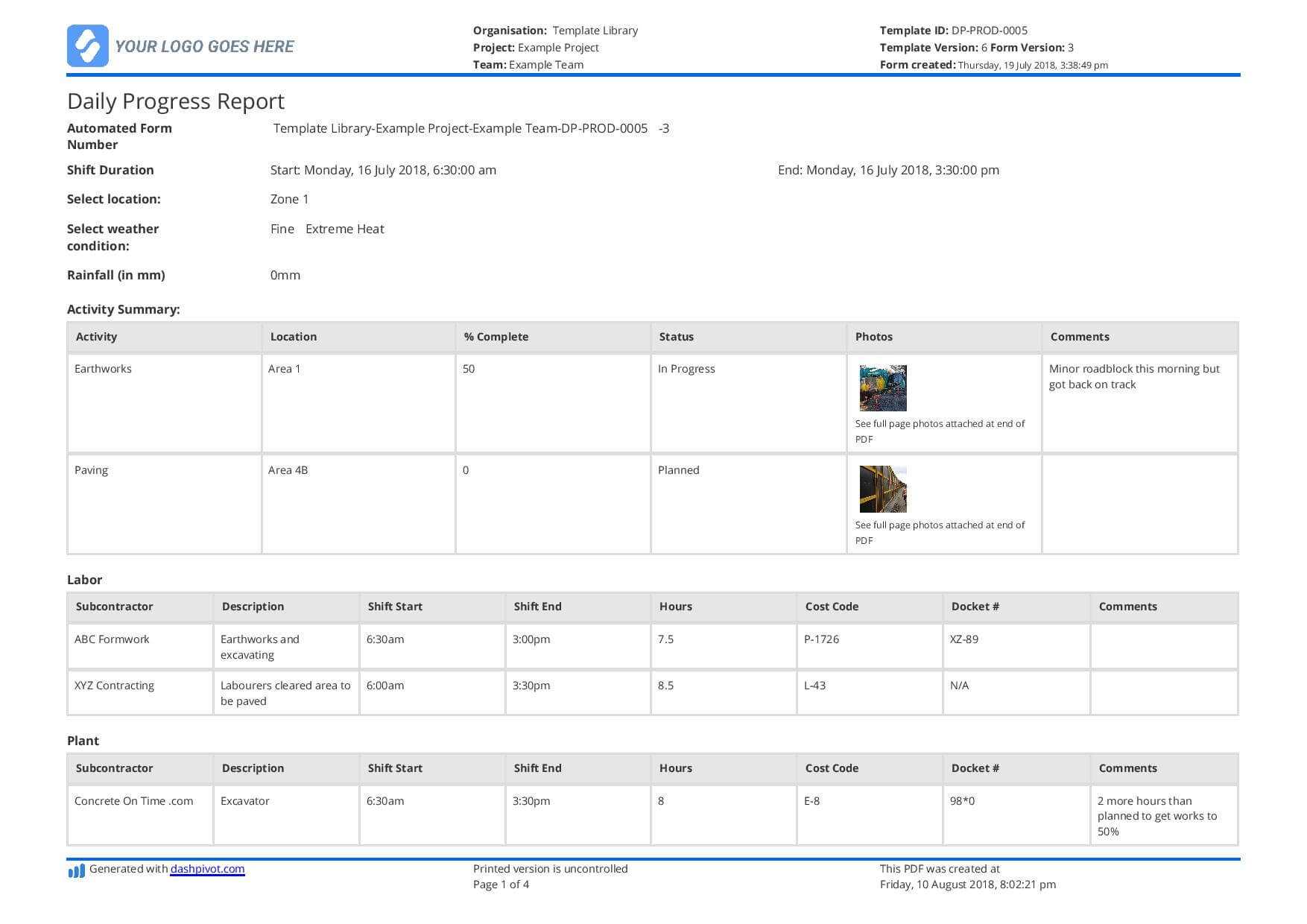
001 Construction Site Daily Progress Report Format Template with Progress Report Template For Construction Project
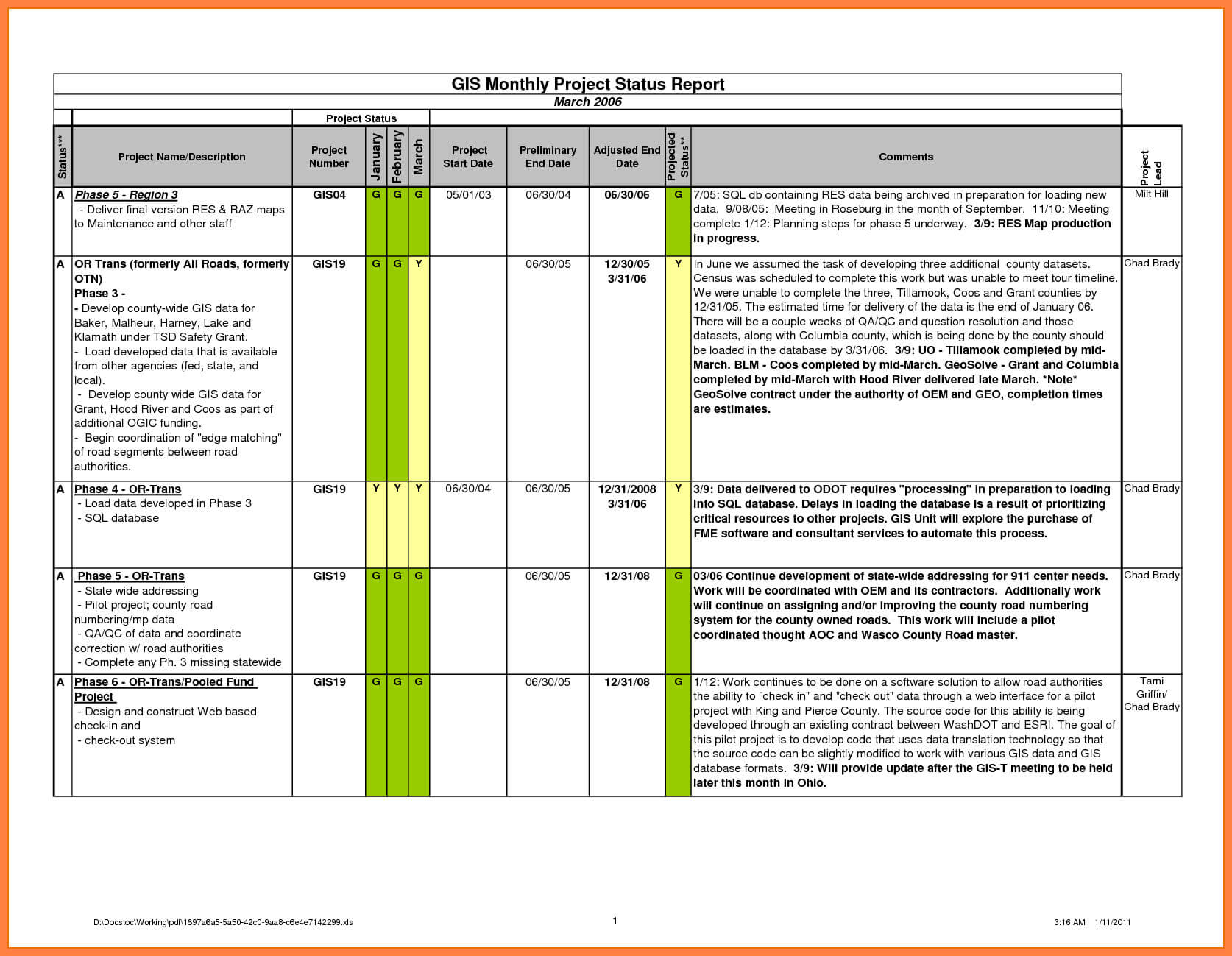
40+ Project Status Report Templates [Word, Excel, Ppt] ᐅ regarding Progress Report Template For Construction Project
018 Template Ideas Construction Site Daily Progress Report with regard to Progress Report Template For Construction Project
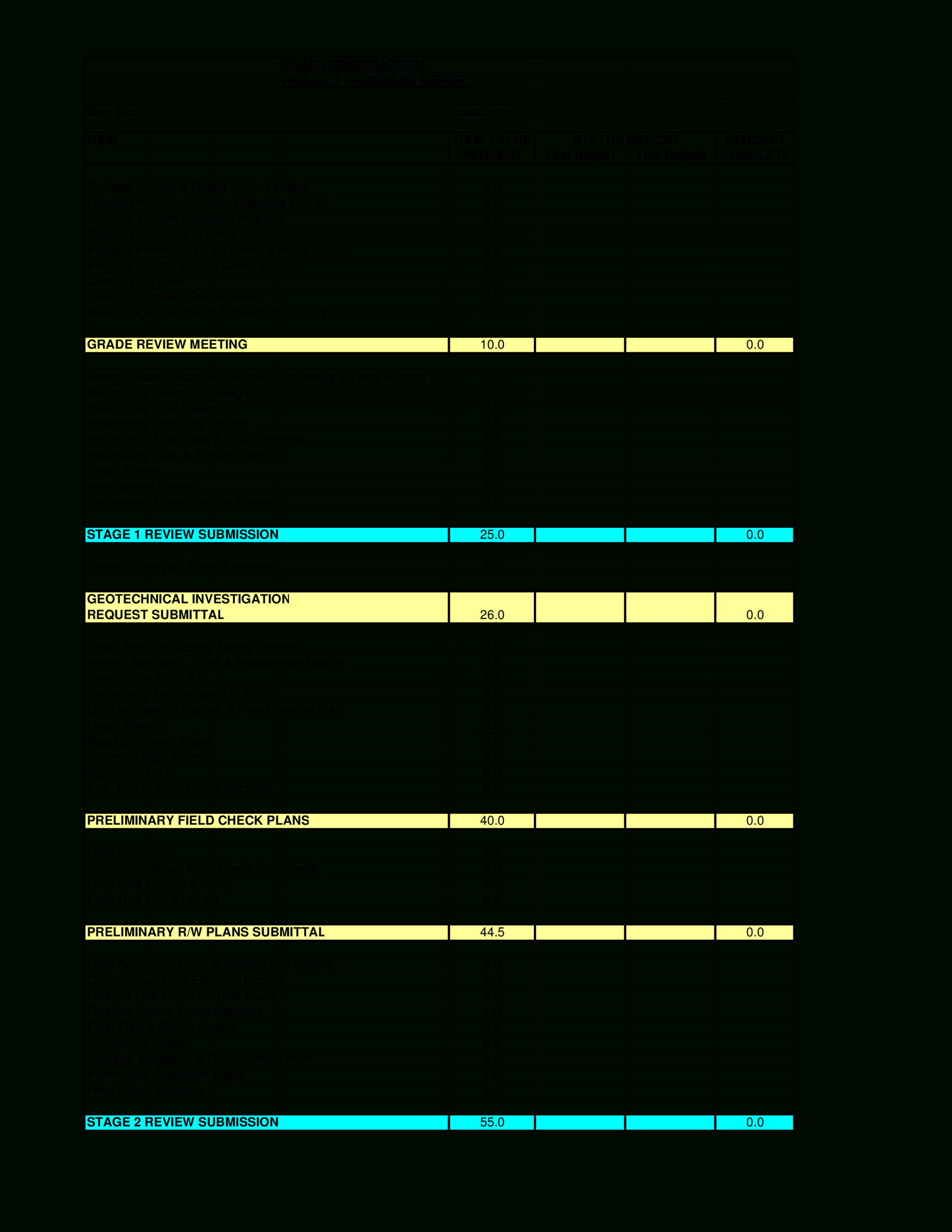
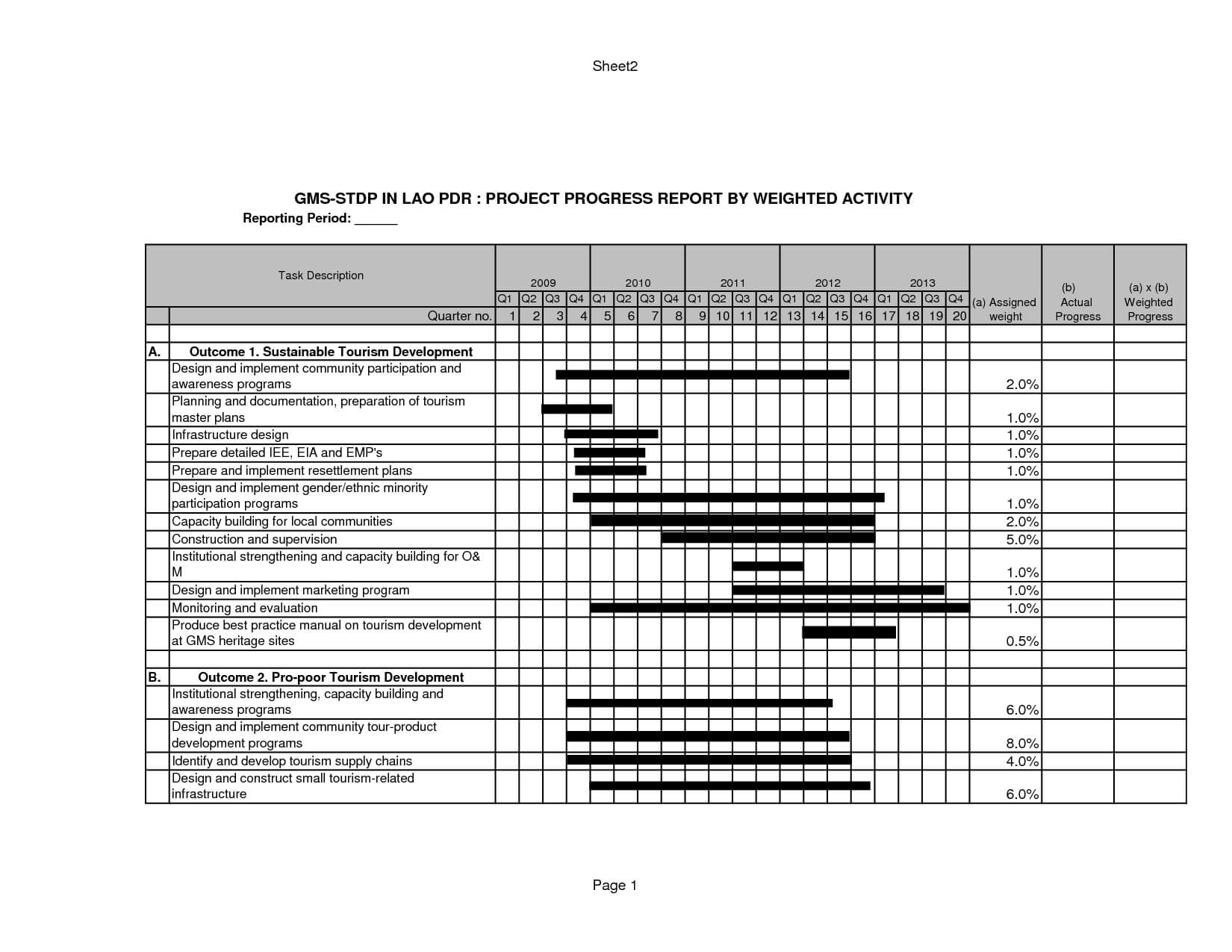
Road Construction Project Progress Report | Templates At within Progress Report Template For Construction Project
023 Best Photos Of Progress Report Template Construction pertaining to Progress Report Template For Construction Project
Free Building Construction Progress Report Sample (Customisable) with Progress Report Template For Construction Project
Monthly Construction Progress Report Template: Use This throughout Progress Report Template For Construction Project